
Understanding Overactive Bladder
Overactive bladder (OAB) can feel frustrating, unpredictable and sometimes embarrassing — but you are not alone, and it is very treatable.
You may experience:
- Urgency (a sudden, strong need to pass urine)
- Frequency (going more often than normal)
- Nocturia (waking at night to pass urine)
- Urge leakage
- Anxiety about being away from toilets
Our structured Overactive Bladder Pathway provides a clear, evidence-based plan to assess, support and improve your symptoms in a calm and compassionate environment.
We follow national best practice guidance and tailor everything to you.
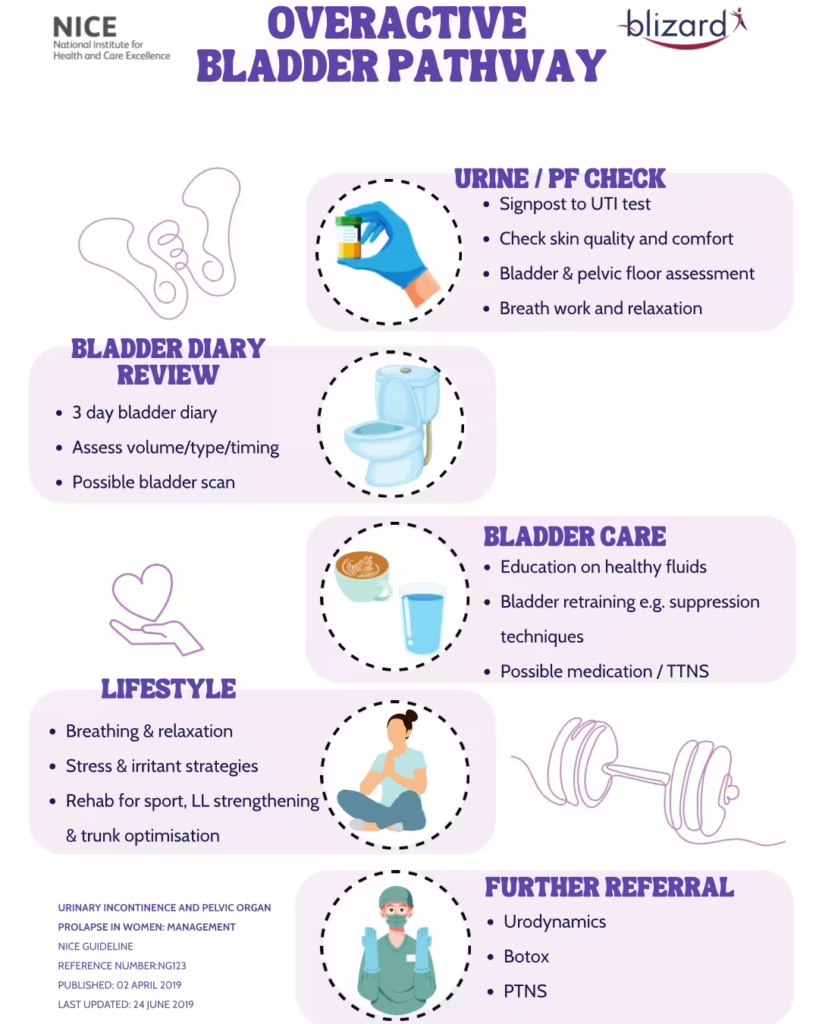
Our Overactive Bladder Pathway
1. Urine & Pelvic Floor Check
Your journey begins with a thorough assessment to understand what is driving your symptoms.
We will:
- Signpost for urine testing to rule out infection (UTI)
- Assess bladder and pelvic floor function
- Check skin comfort and irritation
- Explore breathing patterns and tension
- Identify lifestyle and nervous system influences
This stage ensures we treat the cause, not just the symptoms.
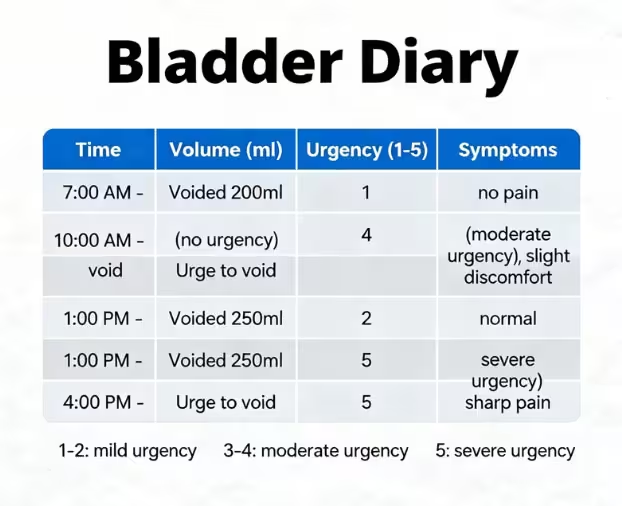
2. Bladder Diary Review
You will complete a simple 3-day bladder diary so we can understand:
- Fluid intake
- Timing of voiding
- Volumes passed
- Leakage episodes
- Trigger patterns
Where appropriate, we may perform a bladder scan to assess residual urine.
This gives us objective information to guide your personalised plan.
3. Bladder Care & Retraining
Education is empowering. We will guide you through:
- Healthy fluid strategies
- Reducing bladder irritants (if relevant)
- Urge suppression techniques
- Bladder retraining to increase capacity
- Pelvic floor coordination work
If needed, we can liaise with your GP regarding medication or discuss options such as TTNS.
The goal is to help your bladder feel calmer, more predictable and more resilient.
4. Lifestyle & Whole-Body Support
Your bladder does not work in isolation.
We look at:
- Breathing and nervous system regulation
- Stress management strategies
- Bowel health
- Lower limb and trunk strength
- Return to exercise and sport
A calm nervous system supports a calm bladder.
5. Further Referral (If Needed)
Most people improve significantly with conservative treatment.
However, if symptoms persist, we can support onward referral for:
- Urodynamics
- Botox
- PTNS
You will always be fully informed and supported in any next steps.
What Makes Our Pathway Different?
- Evidence-based and NICE-informed
- Individualised and holistic
- Focused on long-term control, not quick fixes
- Delivered in a supportive, confidential environment
We aim to give you confidence, control and clarity.

Who Is This Pathway For?
This pathway is suitable for:
- Women experiencing urgency or urge leakage
- Postnatal women
- Peri- and post-menopausal women
- Those with pelvic organ prolapse and bladder symptoms
- Anyone feeling anxious about bladder control
If you’re unsure whether this applies to you, we’re happy to guide you.

What Outcomes Can You Expect?
Many clients experience:
- Reduced urgency
- Fewer toilet visits
- Better night-time sleep
- Improved confidence
- Return to exercise and social activities
Progress is usually seen within 4–8 weeks when exercises and strategies are followed consistently.
Take the First Step
If bladder symptoms are affecting your quality of life, support is available.
Book an initial pelvic health assessment with Blizard Physiotherapy and begin your personalised Overactive Bladder Pathway today.